Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
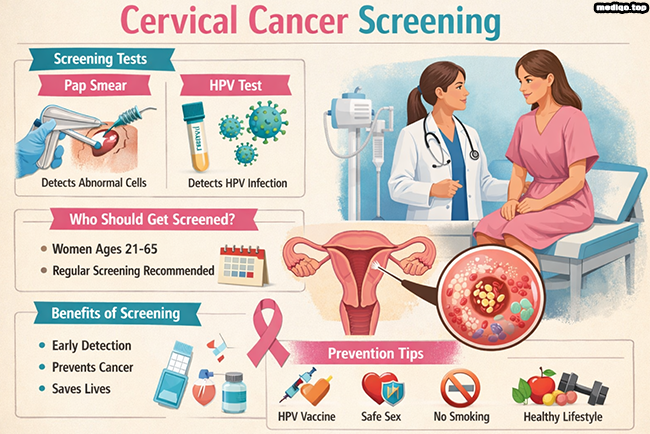
Cervical cancer screening helps detect abnormal cell changes in the cervix before cancer develops. It allows early treatment and prevents serious complications. Cervical cancer remains one of the most preventable cancers with proper screening. Regular testing identifies precancerous lesions and early-stage cancer. Early detection improves survival rates and treatment success. Screening plays a key role in protecting women’s reproductive health. Many women show no symptoms in early stages. Screening ensures problems get identified before symptoms appear. Health organizations strongly recommend routine screening for eligible women. Awareness and timely testing can save lives.
Cervical cancer develops slowly over several years. It begins with abnormal cell changes caused by human papillomavirus (HPV). Most HPV infections resolve naturally, but some persist and cause cancer. Screening detects these abnormal changes early. Early treatment prevents progression into invasive cancer. Women who undergo regular screening have lower cancer risk. Screening also reduces mortality rates significantly. It provides reassurance for women with normal results. It allows early intervention when abnormalities exist. Public health programs emphasize screening to reduce disease burden.
Two main tests help detect cervical cancer early. These tests identify abnormal cells and HPV infection.
The Pap smear detects abnormal cervical cells. A healthcare provider collects cells from the cervix. These cells get examined under a microscope. The test identifies precancerous changes. It helps prevent cancer by detecting early abnormalities. Pap tests remain widely used worldwide. They offer effective and reliable screening. Doctors recommend regular Pap testing for eligible women.
The HPV test detects high-risk HPV types. These viruses cause most cervical cancers. The test identifies infection before cell changes occur. It offers higher sensitivity than Pap smear alone. Many guidelines recommend HPV testing as primary screening. It improves early detection and prevention. Combined testing increases screening accuracy.
Women between ages 21 and 65 should undergo screening regularly. Screening recommendations vary by age and risk factors. Women aged 21 to 29 should get Pap tests every three years. Women aged 30 to 65 should get HPV testing every five years. They can also choose Pap testing every three years. Women with weakened immune systems may need frequent screening. Women with HPV infection require close monitoring. Those who had cervical cancer need continued follow-up. Doctors personalize screening schedules based on individual risk.
The procedure takes only a few minutes. It gets performed in a clinic or hospital. The woman lies on an examination table. A speculum gets inserted into the vagina. It allows access to the cervix. The healthcare provider collects cervical cells using a small brush. The sample gets sent to a laboratory. The procedure causes minimal discomfort. Most women tolerate it well. It does not require anesthesia. Normal activities can resume immediately after testing.
Regular screening offers many health benefits. It detects abnormal cells early, prevents cervical cancer development, reduces cancer-related deaths, allows early and less invasive treatment. It improves survival outcomes significantly. Screening provides peace of mind. It reduces healthcare costs through early intervention, supports long-term reproductive health. It empowers women to take control of their health.
Read more >> Chemotherapy Side Effects: Causes, Symptoms, and Management Guide
Cervical cancer screening remains safe and effective. However, some limitations exist. False positive results may occur occasionally. False negatives can happen rarely. Mild discomfort may occur during sample collection. Minor spotting may occur after testing. Screening does not prevent HPV infection. It only detects abnormalities early. Regular follow-up ensures accurate diagnosis. Doctors recommend continued screening despite limitations.
Women older than 65 may stop screening if results remain normal for many years. Women who had total hysterectomy may not need screening. However, those with cancer history need continued monitoring. Doctors evaluate each case carefully. Personal medical history influences screening decisions. Women should consult healthcare providers before stopping screening. Proper guidance ensures safe and appropriate care.
Screening works best when combined with preventive measures. HPV vaccination reduces cervical cancer risk. Safe sexual practices reduce HPV transmission. Limiting sexual partners lowers infection risk. Regular medical checkups support early detection. Avoiding smoking improves cervical health. Maintaining a healthy immune system helps fight infections. Education and awareness improve screening participation.
Cervical cancer screening remains essential for women’s health. It detects abnormal changes early and prevents cancer. Regular screening improves survival and reduces complications. Pap smear and HPV tests provide effective detection methods. Women should follow recommended screening schedules. Preventive measures enhance screening effectiveness. Early detection saves lives and protects reproductive health.